Lately, several people have pointed out that our family was hit particularly hard by the pandemic. We certainly have had a string of misfortunes, no doubt about that, but it’s hard for me to accept that we were hit hard by the pandemic. After all, no one I know personally has died of COVID—I know families who have lost several people this year, but everyone I know personally who had COVID survived (even a few who were very seriously ill). The families who lost loved ones were hit hard by the pandemic. We have been lucky.
But there can be no denying that several bad things have happened this year. I’m losing my resilience, as the hits keep coming before I even get back up.
First off, I lost my job. This was partly my fault; I knew layoffs were possible and told my executive director that if anyone from my department was laid off it should be me and not my coworkers. I was the new guy, the lowest on the totem pole, and it didn’t seem fair for me to keep my job if others had to lose theirs. And this appears to have worked, because all of my fellow editors are still there.
Then, of course, I lost our family’s health insurance. COBRA was completely unaffordable and I’m not sorry I opted out of that, but I do sometimes wonder why I didn’t try to get a marketplace plan over the summer. It never occurred to me at the time, though it certainly does now. But the reality is that I probably would have opted out then anyway, because we were worried about money and I wouldn’t have thought I could afford the premiums. (I would have been correct about that, too.)
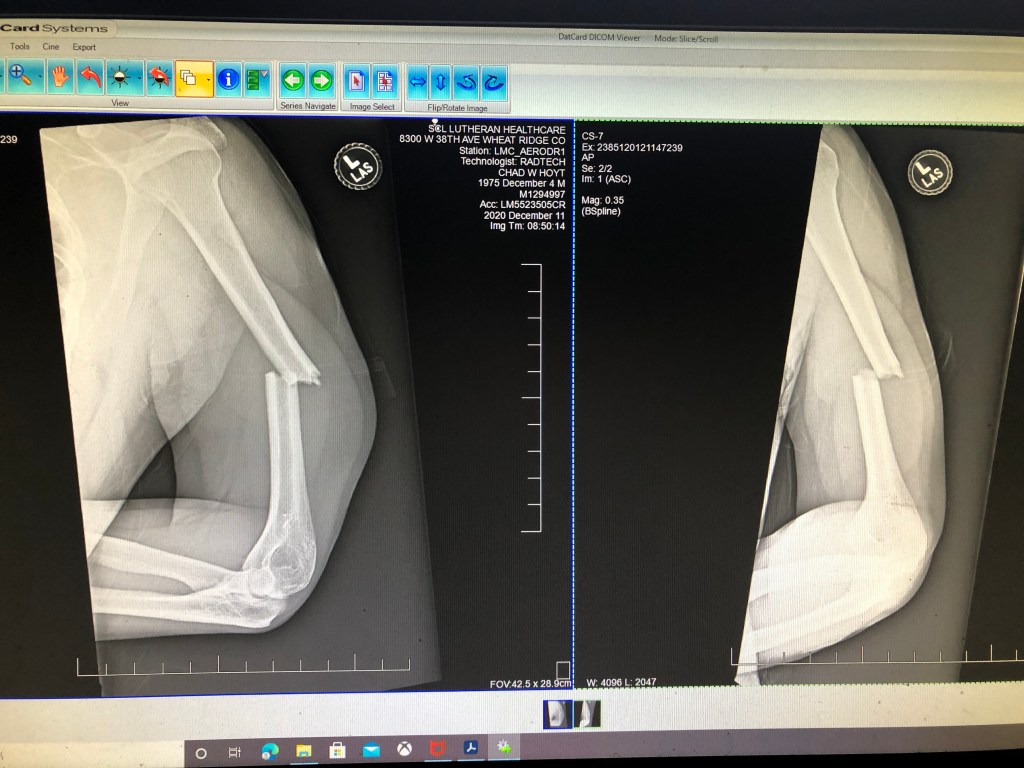
Losing the health insurance wouldn’t have been a problem if Chad hadn’t had his car accident. We were able to pay for the kids’ well visits and our flu shots out of pocket and it wasn’t a huge expense. But man, that car accident is just the gift that keeps on giving. Chad, of course, feels it the most. He is in constant pain, he does not yet have full range of motion, and he can’t even pick up Elliot.
I am dealing with the more administrative side of his accident. I’m dealing with all the medical bills and trying to get the car figured out. Almost every day, I deal with something related to the accident. Lately, it’s all been dealing with State Farm. It’s a very long story, but they aren’t willing to pay for all the damage to the car and they also won’t even allow anyone to assess whether the car is safe to drive. At this point, I’m ready to dump State Farm for good and get rid of the car to whoever wants it, but I can’t because we haven’t reached a resolution of any kind yet.
And then there have been a million other things that have come up, too.
I was supposed to take the skills portion of the CNA licensure test on February 26. My test was at 8 am in Pueblo, which is about 2 hours away from my house, so I got up at 4:45 that morning, got ready, and was in my car at 5:30 am, only to discover it wouldn’t start. I tried for 10 minutes or so to get it started and finally woke up Chad. Together, we tried until about 6:05, when I would have been late for the test anyway. I never did make it to Pueblo that day, and spent the whole day trying to get my car towed to our repair shop, getting a rental car, and also dealing with nasty adjusters regarding Chad’s accident. That was also the day I found out they’re not covering the majority of the damage to Chad’s car. They say it was unrelated. I can’t make them change their mind and they said they would only consider proof that doesn’t exist—pictures of the accident from the day it happened.
I still am not a fully licensed CNA, but thankfully the agency I was working with agreed to keep me despite my failure to test. The test has been rescheduled for 11:30 am next Friday in Pueblo (that facility is the only one offering the skills test at this time, apparently). This was for the job I have been trying to get since July. The only job I *can* get. The only job that allows me to take care of Grace and keep her safe. To miss the test was to jeopardize my only chance at making an income. It wasn’t just a big deal—it was a BIG DEAL. Add to it the $950 repair bill for my car, plus the $350 for the rental, and it was a certifiably bad day.
The latest in the “what else can go wrong” saga is that our washing machine is broken. If we have to replace it, it will be the third major appliance we’ve had to replace this year. It will almost certainly be hundreds of dollars to repair but we’ll find out tomorrow.
It feels like a very long time since we’ve had money to spare for anything. I have been extremely careful about what groceries and household products I buy. I keep having to tell the kids no when they want the latest and greatest toys and in-app purchases, which I hate. I try to only get gas at Costco, where it is considerably less expensive. I downgraded our expenses as much as possible, and yet every time I turn around there’s another hand sticking out, waiting for its due. The financial stress is unbelievable.
And yet, we are the lucky ones. We have family to help us out and give us a safety net when we need it. We have never not been able to buy milk and diapers, thanks to some gift cards friends and organizations gave us. We aren’t literally starving. And most importantly of all, our family is alive and relatively healthy.
There truly have been a lot of things that have gone wrong for us. We have had a lot of hardships since COVID hit. But there are so many things that have gone right, too. We are the lucky ones.